Diabetic Foot Care: Why Seeing a Podiatrist is Important


Michelle DeMarchi
BSc PT, DOMP
Physiotherapist, Pelvic Health Physiotherapist, Bracing Specialist
When it comes to managing diabetes, taking care of your feet is crucial, yet often overlooked. Whether you’re familiar with the term podiatrist or chiropodist, both professionals are key players in diabetic foot care.
With diabetes increasing the risk of foot complications, from minor sores to serious infections, seeing a podiatrist or chiropodist can make all the difference in preserving your mobility and quality of life.
Dive into why expert foot care is not just a recommendation, but a necessity for anyone living with diabetes.
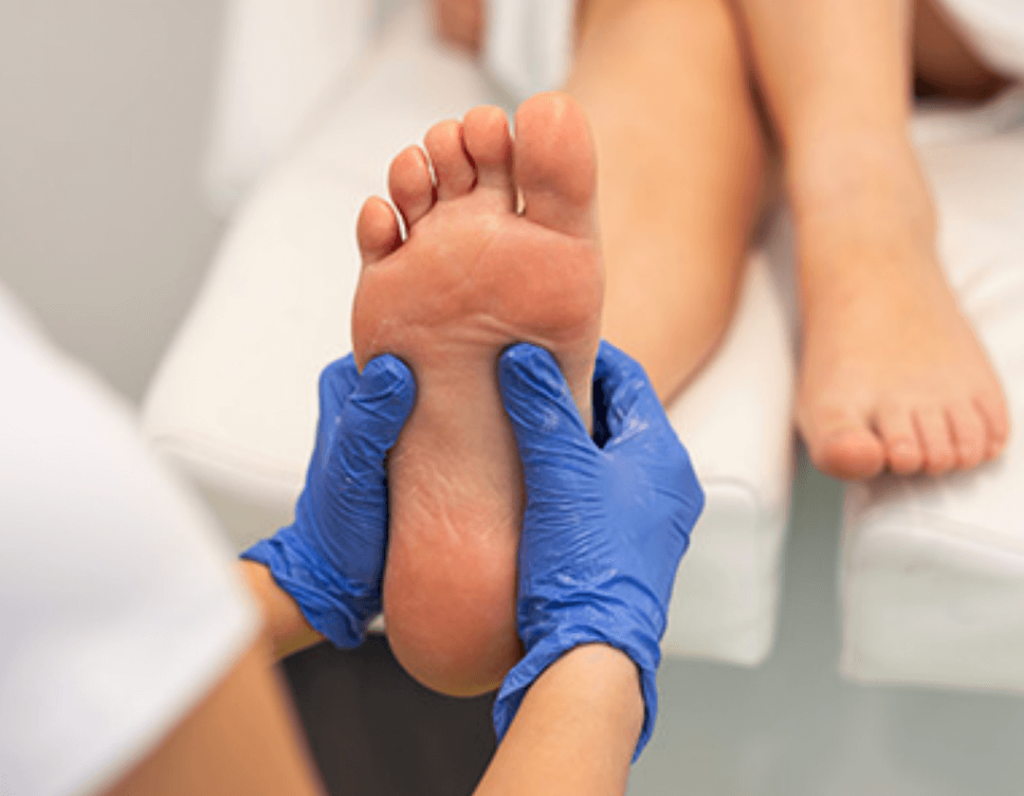
What is diabetic foot care, and why is it important?
Diabetic foot care encompasses a range of practices and treatments aimed at preventing and managing foot complications that can arise as a result of diabetes. People with diabetes are at higher risk for foot issues due to factors such as poor circulation, reduced sensation and an increased likelihood of infections.
Here’s why diabetic foot care is crucial:
1. Early detection of complications: Routine check-ups with a podiatrist or chiropodist can help spot early signs of issues such as neuropathy (nerve damage) or vascular problems, allowing for timely intervention and management
2. Prevention of infections and ulcers: High blood sugar levels can impair wound healing and diminish the skin’s ability to fight infections. Regular foot inspections and proper care can help identify and treat minor issues before they develop into serious ulcers or infections.
3. Reduced risk of amputation: Diabetes can lead to severe complications like gangrene, which may result in amputation if not managed promptly. By maintaining good foot care, the risk of such extreme measures can be significantly reduced.
4. Maintain mobility and function: Foot problems can lead to pain and difficulty walking, impacting overall mobility and quality of life. Effective foot care helps prevent discomfort and maintain an active lifestyle.
5. Advice, education and guidance: Diabetic foot care often involves learning how to properly care for your feet, including proper nail trimming, choosing appropriate footwear, and recognizing warning signs of potential problems. Podiatrists and chiropodists provide valuable education and guidance to help patients manage their condition effectively.
In essence, diabetic foot care is about proactive management to prevent serious complications and maintain overall foot health, ensuring a better quality of life for those living with diabetes.
How does diabetes affect foot health and what are common foot problems?
Diabetes affects foot health in several significant ways, primarily through its impact on circulation and nerve function.
1. Peripheral neuropathy (nerve damage): High blood sugar levels can damage the nerves in the feet, leading to peripheral neuropathy. This condition reduces sensation, making it difficult to feel injuries, blisters, or infections. Without proper sensation, minor wounds can go unnoticed and become severe.
2. Poor Circulation: Diabetes can impair blood flow to the feet due to damage to the blood vessels. Reduced circulation slows down the healing process of wounds and increases the risk of infection. It can also lead to a condition called peripheral artery disease (PAD), which further exacerbates poor blood flow.
3. Increased risk of infections: Elevated blood sugar levels can weaken the immune system and reduce the body’s ability to fight infections. Small cuts or blisters can quickly become infected and may not heal properly, leading to serious complications.
4. Foot ulcers: Chronic high blood sugar can cause damage to the skin and underlying tissues, leading to foot ulcers. These open sores are common in people with diabetes and can become serious if not treated promptly. They often occur on areas of the foot that experience pressure or friction.
5. Charcot foot: This is a condition where the bones in the foot become weakened and break due to nerve damage. It can cause the foot to change shape, leading to deformities and increased risk of ulcers and infections.
6. Fungal and bacterial infection: Diabetes can make individuals more susceptible to fungal infections (such as athlete’s foot) and bacterial infections, further complicating foot health.
7. Dry and cracked skin: Reduced blood flow and neuropathy can lead to dry, cracked skin on the feet. Cracks in the skin can serve as entry points for infections.

8. Deformities and pressure points: Diabetes can lead to changes in foot structure, such as bunions or hammertoes, which can create pressure points and increase the risk of ulcers and pain.
Overall, diabetes can lead to a range of foot problems that require vigilant care and management. Regular check-ups with a healthcare professional, such as a podiatrist or chiropodist, are essential for monitoring foot health and preventing complications.
How can a podiatrist or chiropodist help prevent diabetic foot problems?
A podiatrist or chiropodist plays a crucial role in preventing diabetic foot problems through a combination of regular assessments, personalized care, and education.
Routine Foot Exams
Regular check-ups with a podiatrist or chiropodist can help catch potential issues early. They conduct comprehensive foot examinations to detect signed of neuropathy, poor circulation or developing ulcers before they become serious.
Wound Care and Treatment
If you develop foot ulcers or infections, these specialists provide expert treatment to promote healing and prevent complications. They can debride (remove) dead tissue, apply appropriate dressing and prescribe medication to manage infections.
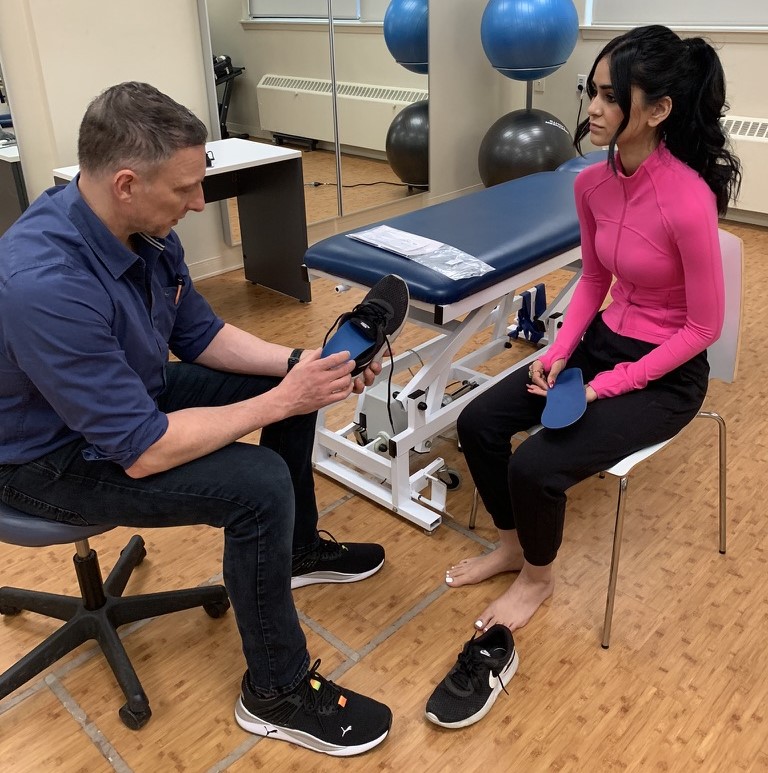
Footwear Advice
Proper footwear is vital for people with diabetes to prevent pressure sores and injuries. Podiatrists and chiropodists can recommend or prescribe custom orthotics and properly fitted shoes to reduce pressure points and provide support.
Nail Care
Regular nail trimming and management are essential to avoid ingrown toenails and infections. These specialists can perform nail care and teach you the correct techniques for maintaining healthy nails at home.
Education and Guidance
They provide education on proper foot care practices, including how to inspect your feet daily, how to avoid common foot problems, and the importance of maintaining good blood sugar control.
Managing Foot Deformities
If you have foot deformities like bunions or hammertoes, a podiatrist or chiropodist can offer treatment or recommend surgical options to correct or alleviate these issues, which can help prevent complications.
Customized Treatment Plans and Foot Health Monitoring
Based on individual needs, they create personalized care plans to address specific risks or conditions related to diabetes, ensuring that each patient receives the most effective care. They will also provide ongoing monitoring to help manage and prevent complications, ensuring that any changes in foot health are promptly addressed.
By working closely with a podiatrist or chiropodist, individuals with diabetes can take proactive steps to safeguard their foot health, minimize the risk of serious complications and maintain a higher quality of life
Why is regular foot screening important for people with diabetes?
Regular foot screening is vital for people with diabetes because it helps identify potential issues early, preventing minor problems from escalating into serious complications.
Diabetes increases the risk of foot issues due to nerve damage and poor circulation, making it difficult to detect problems until they become severe. Screening allows for early detection of ulcers, infections and circulation issues. This enables timely intervention and reduces the risk of severe outcomes such as amputations.
Additionally, foot screening helps manage diabetic neuropathy by assessing nerve health and loss of sensation, ensuring that unnoticed injuries are addressed. They also provide opportunities for healthcare professionals to offer education on proper foot care, recommend appropriate footwear and orthotics and develop personalized care plans.
Overall, regular screenings are a proactive approach that contributes to maintaining foot health and improving quality of life for individuals with diabetes.
Click here, to continue to learn more about diabetic foot screens!

What signs of foot problems should diabetics look out for?
Diabetics should be cautious of several key signs of foot problems, as early detection is crucial for preventing diabetic neuropathy, which can impair sensation and lead to unnoticed injuries.
1. Unusual sensations: Numbness, tingling or a “pins and needles” feeling in the feet can indicate diabetic neuropathy, which can impair sensation and lead to unnoticed injuries.
2. Pain or discomfort: Persistent or worsening pain in the feet, especially if it is accompanied by swelling or redness, may signal issues like infections, ulcers or Charcot foot.
3. Changes in skin colour: Look for changes in skin colour, such as redness, blueness or paleness, which can suggest circulation problems or infections.
4. Swelling: Unexplained swelling in the feet or ankles may indicate fluid retention, infections or vascular issues.
5. Foot ulcers or sores: Any open sores, blisters or ulcers on the feet that do not heal or are slow to heal can become serious if not treated promptly.
6. Dry or cracked skin: Excessively dry, cracked skin can lead to infections and should be addressed with proper moisturizing and care.
7. Changes in foot shape: Noticeable changes in foot shape, such as swelling, deformities, or lumps may be signs of structural issues or complications like Charcot foot.
8. Nail issues: Ingrown toenails, fungal infections or other abnormalities in toenails should be monitored and treated to prevent further problems.
9. Wounds or cuts: Any cuts, scratches or injuries that seem to be worsening or not healing properly need immediate attention.
How often should someone with diabetes see a podiatrist or chiropodist?
People with diabetes should generally see a podiatrist or chiropodist at least once a year for a comprehensive foot exam. This annual visit helps monitor foot health, identify any complications early, and receive advice on maintaining proper foot care.
For individuals with existing foot problems, such as ulcers or severe neuropathy, more frequent visits – every 3 to 6 months – might be recommended to manage and prevent complications effectively.
High-risk patients, including those with a history of foot issues, poor circulation or significant neuropathy, may need to see a podiatrist more often. Additionally, if new symptoms such as pain, swelling or sores arise, it’s important to schedule an appointment promptly, regardless of your last visit. Your podiatrist will tailor the frequency of visits based on your specific needs and health status.
How can custom orthotics benefit diabetic patients?
Custom orthotics can be very beneficial for diabetic patients, particularly those with diabetic neuropathy or poor circulation, as they prevent complications related to the feet.
Pressure Redistribution
Diabetic patients often have areas of increased pressure on their feet due to changes in foot structure or abnormal gait. Custom orthotics redistribute pressure across the foot more evenly, helping prevent ulcers and sores from forming high-pressure areas.
Protection Against Ulcers
People with diabetes are prone to developing ulcers due to decreased sensation in their feet. Orthotics can reduce friction and shear forces on the skin, minimizing the risk of foot ulcers, which are a common complication that can lead to serious infection or even amputations.
Support and Stability
Diabetes can lead to changes in the shape of the foot, such as collapsed arches or deformities like Charcot foot. Custom orthotics provide the necessary support to maintain proper foot alignment, offering better stability and reducing the risk of falls or further foot deformities.
Improved Comfort and Functionality
Many diabetic patients experience discomfort when walking due to changes in their foot mechanics. Orthotics can improve comfort, making it easier for patients to maintain their mobility and engage in physical activity, which is crucial for managing blood sugar levels.
Injury Prevention
For patients with neuropathy (nerve damage), orthotics act as a protective barrier, reducing the likelihood of injuries that the patient might not feel due to loss of sensation. They help conditions like blisters, cuts and calluses, which could otherwise go unnoticed and lead to infections.
Custom orthotics play an essential role in diabetic foot care, reducing the risk of complications and improving overall foot health. Click here, to continue learning more!
TAKE CONTROL OF YOUR FOOT HEALTH TODAY!
If you have diabetes, your feet need extra care, and seeing a podiatrist of chiropodist is a key step to achieve this! Schedule your appointment today and take a step toward better foot health!
This blog was written by Francesca Biondi, a Physiotherapy student at the University of Toronto
Frequently Asked Questions
How does proper footwear help in managing diabetic foot care?
Proper footwear is crucial for managing diabetic foot care because it helps prevent pressure sores and ulcers by redistributing pressure evenly across the foot. It also protects against injuries like cuts and blisters, which people with diabetes are more prone to due to decreased sensation. Additionally, supportive footwear helps maintain proper foot structure, reducing the risk of complications like foot deformities.
What are the risks of not treating foot issues in diabetics?
Not treating foot issues in diabetics can lead to severe complications, including the development of ulcers, infections and potentially gangrene, which can result in the need for amputation. Untreated foot problems can also lead to poor wound healing, severe infections and decreased mobility, all of which can significantly impact overall health and quality of life.
Why is regular foot screening important for people with diabetes?
Regular foot screening is crucial for people with diabetes because it helps detect early signs of complications like ulcers, infections and deformities before they become serious. Since many diabetics experience reduced sensation due to neuropathy, they may not feel injuries or changes in their feet, making screening essential for identifying issues that could otherwise go unnoticed. Early detection through regular screening allows for timely intervention, reducing the risk of serious complications such as infections, amputations and mobility loss.
